What Health Conditions Rely On Ventilators?
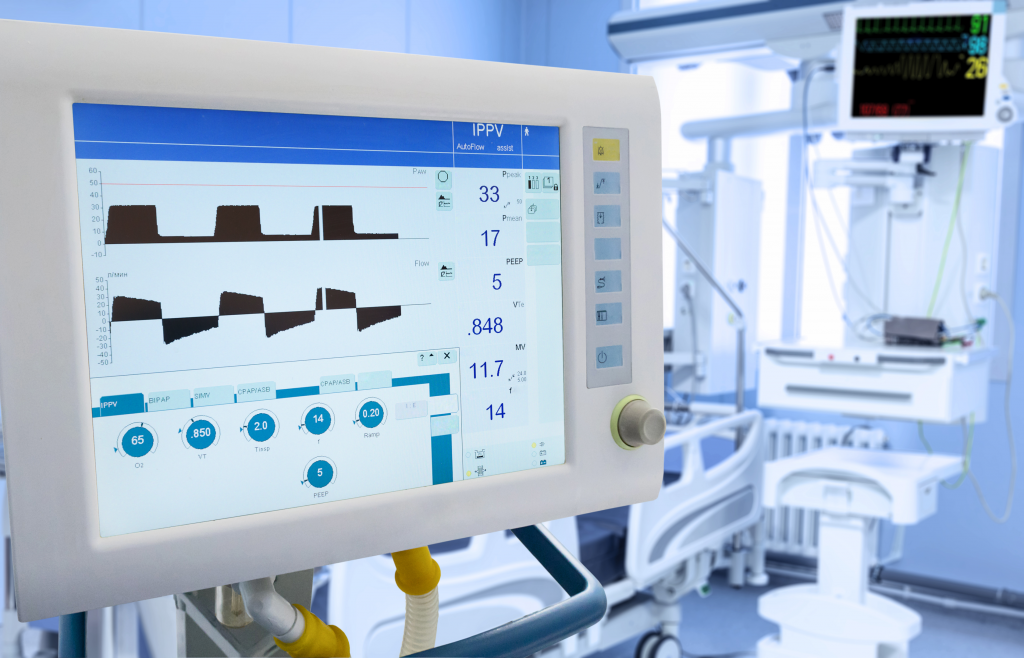
Medical ventilators are life-saving devices that support lung function in order to help a patient breathe. This critically important medical equipment offers invaluable assistance when a patient’s lungs are severely affected because of a health condition and they are struggling to breathe naturally. Ventilators work by pushing air in and out of the lungs, so your body gets the oxygen it requires to keep functioning. The respiratory therapist may either place a fitted mask on your mouth or insert a breathing tube down the throat.
Medical Conditions Where Ventilators Can Help
Respiratory failure is a life-threatening emergency in which the patient is unable to breathe properly on their own. The heart, liver, kidneys, and brain, among other organs, need enough oxygen to be able to function properly. A medical ventilator can provide the oxygen required by different organs to function properly.
Patients with severe lung complications resulting from Covid-19 infection can greatly benefit from ventilator support in many cases. There are a number of other health conditions that may also cause patients to experience breathing issues, and use of a ventilator can help.
Acute respiratory distress syndrome (ARDS)
ARDS is a fast-moving condition that affects critically ill patients. The main challenge faced by respiratory therapists is to prevent fluid from leaking into the lungs of patients. Fluid in the lungs can make breathing difficult or impossible. Most patients with ARDS need to be placed on mechanical ventilators or life support machines by a certified respiratory therapist.
Fluid in the lungs can make it difficult to breathe, resulting in low oxygen levels. This condition is also known as hypoxemia, which can be overcome through oxygen therapy. Respiratory failure occurs when there is increased working of the lungs but low oxygen levels in the body.
A respiratory therapist would be expected to care for patients with ARDS by placing them on ventilator support until their lungs heal. Few patients may also suffer from scarring in the lung if the fluid and inflammation levels increase. This is known as the fibrotic stage of ARDS. This is a highly dangerous stage and requires immediate respiratory care. The lung can deflate or pop, leading to pneumothorax or a collapsed lung condition.
Head injury or stroke
Patients with acute brain injury (ABI) are not placed on ventilator support because they suffer from lung disease – but because they experience decreased respiratory drive. These patients are frequently admitted to the intensive care unit or ICU if they experience respiratory failure because of loss of airway protective reflexes. Respiratory therapists work to ensure that patients are not at risk of developing cardiopulmonary disorders, such as acute respiratory distress syndrome (ARDS) or pneumonia.
Patients with acute brain injury require mechanical ventilation if they experience central respiratory depression because of the primary injury. Lung function, in such patients, can be near normal levels. Pertaining to this, a registered respiratory therapist will still place the patient on mechanical ventilation. The same holds true for patients that experienced a stroke or a traumatic injury to the spine, chest, or abdomen.
Medical professionals perform a series of diagnostic procedures before recommending ventilators. Positive pressure ventilation is usually deemed necessary in cases of neurogenic pulmonary edema. Furthermore, therapies used for managing acute head injury and stroke, such as sedation, paralysis, and barbiturates, can result in central respiratory depression and breathing problems, necessitating mechanical ventilation.
Asthma
Asthma is one of the most common afflictions studied in respiratory therapy. Asthma affects almost 10% of the population, with 11,000 patients dying of it each year. Since 1980, the rate of asthma deaths has witnessed an increase of 50%. By providing competent emergency care and managing ventilators, most asthma deaths can be prevented.
In general, intubation is only appropriate in the ER and critical care units. However, most respiratory therapists will not hesitate to intubate if the patient is crashing. The RT will need to assess lung capacity and carefully evaluate the risks and benefits. Medical facilities generally place a patient suffering from asthma on a ventilator when medication has failed, and there are indications of severe hypoxia.
Acute asthma exacerbation is the primary indication to place a patient on mechanical ventilation. This is a condition characterized by insufficient alveolar ventilation or oxygenation. The decision to place a patient on mechanical ventilation should depend on the lung capacity, pulmonary function tests, degree of respiratory difficulty, and other clinical evaluations.
Indications of hypercapnia and hypoxemia should also be considered when weighing the suitability of ventilatory support for an asthmatic patient. it’s vital to ensure that patients breathe easily. Mechanical ventilation, intubation, and other life support systems should not be delayed if the patient needs them.
COPD (chronic obstructive pulmonary disease) or other lung diseases
COPD, or chronic obstructive pulmonary disease, is an umbrella term for lung diseases that gradually progress and affect a patient’s ability to breathe properly. It commonly consists of emphysema and chronic bronchitis. COPD can make it increasingly difficult to inhale and exhale as it progresses. The condition can require pulmonary rehabilitation in severe instances.
Oxygen levels in the blood can become too low in patients suffering from COPD. Respiratory therapy programs for patient care usually involve oxygen therapy. This can be through oxygen concentrators or oxygen tanks. Physicians usually treat patients with COPD by increasing their oxygen levels to support organ function.
In severe cases, mechanical ventilation may be required to stabilize oxygen and carbon dioxide levels in the body. It’s vital to educate patients and their families on all available treatment options. Healthcare staff can be advised to teach the family members about human anatomy and how artificial airway devices can improve breathing.
Non-invasive ventilation (NIV) makes use of pressurized room air. This is delivered through a mouthpiece or mask to make inhalation easier. COPD patients may need to be admitted to intensive care units. Ventilation makes use of no pressure or lower pressure to help patients exhale carbon dioxide from the body. Doctors may advise patients to use both oxygen therapy and mechanical ventilation as and when necessary.
Cardiac arrest
Cardiac arrest causes a patient to become unconscious, have no pulse, and stop breathing. Cardiopulmonary resuscitation is necessary when this happens to get the heart started as soon as possible. Brain cells start to die within 3 minutes when not receiving oxygen. Soon, other vital organs begin shutting down as well.
Patients have a better chance of recovery if the heart can be started quickly. A patient’s recovery also depends on whether the heart is able to pump again and on general overall health. Treatment provided in the ICU can be complex or straightforward. This depends on the individual situation. Many patients remain unconscious after suffering a cardiac arrest, while others require ventilation and intubation.
Protective ventilation through low tidal volume ventilation can be useful in decreasing pulmonary dysfunction and improving the outcome. The ventilator can provide enough oxygen to the heart to keep it beating. Based on this, incorrect ventilation can increase mortality in both in-hospital and pre-hospital settings. It’s crucial that proper care is taken while treating patients.
Drug overdose
Patients who overdose on prescribed and illegal drugs form a small percentage of those placed on ventilator support. Treatment for these patients ranges from requiring a stomach pump to being immediately intubated. Often, pre-hospital personnel or those in emergency rooms need to take a call regarding the treatment.
Ventilation is usually required when the cardiopulmonary system shuts down. You don’t need to place an overdose patient on mechanical ventilation just because they are experiencing trouble breathing. Complications can arise, including ventilator-induced pneumonia, if the mechanical ventilation is not correctly managed.
Patients that present a drug overdose are usually ineffective in maintaining spontaneous breathing. All drugs can result in respiratory depression if ingested in sufficient quantity. This can require mechanical ventilation. Sometimes, patients with drug overdose are also intubated for airway protection. Regurgitation and aspiration are two major concerns in patients on ventilation. The endotracheal tube cuff should be adequately inflated.
Neonatal respiratory distress syndrome
This is a breathing problem that can affect newborns, especially premature infants. RDS, or neonatal respiratory distress syndrome, usually presents in newborns within a few hours after birth. Pre-term neonates are the most affected by this condition. In most cases, the infant needs to be placed in a neonatal intensive care unit.
Treatment modalities include advanced respiratory care, antenatal corticosteroids, and surfactants. It’s essential to note that even in skilled nursing facilities with some of the top neonatal intensive care units, mortality and morbidity in pre-term infants run high. Assisted ventilation is usually recommended in RDS to provide a constant distending positive airway pressure.
The early initiation of continuous positive airway pressure (CPAP) is a preferred strategy. Ventilation with selective surfactant administration is also recommended. Non-invasive modalities are typically preferred over invasive ventilation in premature babies. This helps in decreasing the risk of bronchopulmonary dysplasia (BPD) and mortality as compared to invasive ventilation.
Pneumonia
Mild pneumonia generally doesn’t need a trip to the emergency room. It can be easily treated at home with antibiotics and rest. This is if the pneumonia is caused by a bacterial infection. In severe cases, you may need to visit a hospital. Sometimes, prolonged stays in nursing homes and other healthcare facilities may also result in pneumonia.
Pneumonia is the most common precursor to acute respiratory distress syndrome (ARDS). You may need invasive ventilation if your pneumonia is not responding to medication and renders you unable to breathe. Patients may also need to be admitted to an intensive care unit.
Learn More About the Benefits of Medical Ventilators: Join an Online Continuing Education Course at TheCEPlace
TheCEPlace is a leading course provider of continuing education units for respiratory therapists. You can obtain the CE credits required for license renewal while adding to your skills and knowledge. Healthcare employers prefer their respiratory therapists to have updated knowledge about the latest techniques and developments in the field of respiratory therapy.
The courses are based on topics that are in high demand, such as the effect of air pollution on blood samples, chest physiotherapy, lung cancer, sleep disorders, and other clinical components. The courses are offered in a simplistic and easy-to-understand manner that will also help you enhance your problem-solving skills and interpersonal skills. All courses offered by TheCEPlace are approved by the main certifying body – American Association for Respiratory Care (AARC)
TheCEPlace has helped countless respiratory therapists get the information and skills needed to further their careers. Get started on your continuing education units today by calling us at 833-388-2600 or register with us online.